Cosmetic Dentistry
Teeth Whitening and Sensitivity: What's Actually Happening Inside Your Teeth
Teeth whitening is safe for most people when used correctly, but the "zingers" and sensitivity you feel aren't random — they follow a specific biological process involving fluid movement inside your teeth. Understanding why sensitivity happens, and how OTC products differ from professional teeth whitening treatments, helps you make smarter choices before you whiten.
Why Whitening Causes "Zingers" — And Why It's Not Nerve Damage
The sharp, sudden pain people describe after whitening — those electric "zingers" — consistently alarm my patients more than anything else. For Cypress-area patients, the good news is: in the vast majority of cases, this isn't nerve damage. It's fluid mechanics.
Here's the biology. Your teeth aren't solid. Beneath the enamel lies dentin, a tissue riddled with microscopic channels called dentinal tubules that run straight toward the pulp. Hydrogen peroxide, the active ingredient in virtually every whitening product, has a low molecular weight that lets it diffuse rapidly through enamel and into those tubules. Research published in PMC describes this as the hydrodynamic mechanism: peroxide temporarily dehydrates the tubule fluid and widens the tubule openings, causing rapid fluid movement that stimulates the nerve receptors at the pulp. Your brain interprets that fluid shift as pain — not because tissue is destroyed, but because those receptors are doing exactly what they're designed to do.
This is also why sensitivity is temporary. Once you stop applying the whitening agent, your saliva begins remineralizing the enamel and the tubule "plugs" rehydrate naturally. According to Cleveland Clinic, this sensitivity is common and transient. But waiting it out passively isn't your only option.
A targeted rehydration protocol speeds recovery considerably. I recommend patients use a neutral sodium fluoride gel or a hydroxyapatite-based toothpaste immediately after each whitening session. Both work by physically depositing mineral into the open tubule entrances, essentially re-plugging them and interrupting the fluid movement that causes pain. Potassium nitrate, found in many sensitivity toothpastes, works differently — it depolarizes the nerve itself, reducing its ability to fire. Using these products before whitening sessions can blunt sensitivity before it starts.
Patients with existing gingival recession are at higher risk. A study cited on PubMed found a statistically significant correlation between gingival recession and whitening sensitivity, since exposed root surfaces lack the enamel layer that otherwise slows peroxide penetration.
The Hidden Risk Nobody Warns You About: Existing Fillings and Bonding
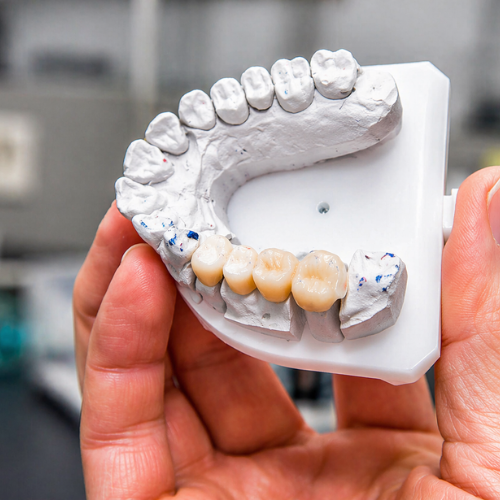
Most online guides mention that whitening won't change the color of crowns or fillings. What they skip is something more concerning: high-concentration peroxide can actively degrade the interface between your tooth and an existing composite resin restoration.
This matters especially for Class V restorations — cavity fillings placed at the gum line to repair decay or cover sensitive root surfaces. These margins are already under mechanical stress. When concentrated peroxide contacts an older or slightly worn composite margin, it can cause micro-gaps to open at the bond between tooth and filling. The whitening agent then seeps underneath the restoration, reaching unprotected dentin directly. The result is a localized, intense sensitivity that feels different from typical whitening sensitivity — sharper, more persistent, and confined to one tooth.
This is one of the most concrete reasons I conduct a thorough exam before any whitening treatment. It's not a sales step. I'm looking at the integrity of every restoration margin, particularly near the gumline, to identify restorations that should be replaced before whitening begins. If you're using OTC kits at home and you have older dental bonding or composite fillings, this is a risk worth discussing with your dentist first.
The pH Problem With Budget OTC Kits
When patients ask whether OTC whitening products are safe, the conversation usually centers on peroxide percentage. That's the wrong variable to focus on. The more important factor — and the one almost never printed on the box — is pH.
Professional whitening gels are formulated with buffering agents that maintain a near-neutral pH. This means the peroxide does its job through oxidation: breaking down the chromogen molecules (the colored compounds) inside and on the tooth surface without chemically etching the mineral structure. The ADA notes that properly used peroxide-based products are considered safe and effective for this reason.
Many budget OTC strips and pens, particularly those marketed through social media, use acidic formulas. The low pH etches the enamel surface to accelerate whitening. This produces faster visible results, but the trade-off is real: acidic etching removes mineral content, alters enamel surface morphology, and makes teeth more permeable to restaining. The ADA News has warned that regular bleaching without professional oversight can result in enamel erosion that salivary remineralization cannot fully reverse.
When evaluating any OTC product, look beyond the peroxide percentage. If the product doesn't list a pH or disclose its buffering system, that's a meaningful gap. Products carrying the ADA Seal of Acceptance have met safety and efficacy standards — that's the most reliable shortcut for patients choosing between options. Mayo Clinic recommends consulting your dentist before starting any bleaching regimen, especially if you have sensitive teeth, recession, or restorations.
Is Professional Whitening Safer for Your Gums?
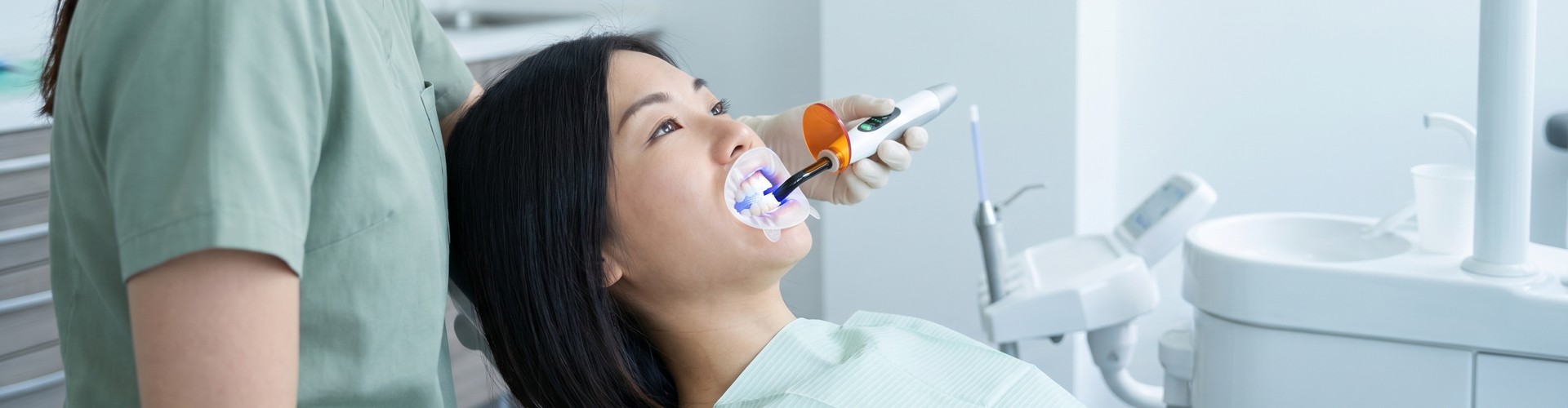
In-office whitening uses higher peroxide concentrations — typically 25% to 40% hydrogen peroxide — which raises a fair question about gum safety. The short answer is yes, professional treatment is generally safer for your gums, and the reason is control.
In a clinical setting, I apply a light-cured resin barrier to the gingival tissue before placing any whitening agent. This isolates the gel entirely to the enamel surfaces. Without that barrier, concentrated peroxide contacts soft tissue directly, causing chemical irritation or even localized burns. This is why gum disease irritation rates are higher with in-office treatment in studies where barrier protocols are inconsistent — the peroxide, not the procedure itself, is the variable.
At-home trays dispensed by a dentist occupy a middle ground. The custom fit minimizes gel overflow onto the gums, and the carbamide peroxide concentration (typically 10–16%) releases hydrogen peroxide more slowly than in-office gels. This slower release reduces peak tissue exposure. The whitening effect is more gradual, but the side effect profile is gentler.
For most healthy adults with intact enamel and no significant recession, professional whitening once or twice a year is well within safe parameters. The whitening effect from a single course can last well beyond a year with reasonable dietary habits.
Ready to Whiten Safely? Talk to Us First.
If you're in Cypress or the surrounding North Orange County area and considering teeth whitening, I'd encourage you to start with a conversation rather than a drugstore purchase. A brief cleaning and exam tells us whether your enamel, gums, and existing restorations are ready for whitening — and which method will give you the best results with the least sensitivity.
Cypress Family Dental offers professional whitening options tailored to your specific tooth structure and goals. Reach out to schedule a consultation — we're here to help you get the result you want, safely.
Medical disclaimer: This article is for informational purposes only and does not constitute professional dental advice, diagnosis, or treatment. Always consult a qualified dental professional before beginning any whitening regimen, particularly if you have existing dental restorations, gingival recession, or a history of tooth sensitivity.








..png)




..png)













